
Chronic Venous Insufficiency: Know What to Look for – and How It’s Diagnosed

Everybody knows the heart plays a central role in circulation, pumping blood throughout the body to provide organs and tissues with oxygen and essential nutrients. But few know the heart has a little help, especially once the first “half” of the circulatory cycle is complete and the blood needs to travel from the extremities and back to the heart. That’s when tiny valves inside the veins help out, opening and closing in rapid succession to create a kind of current that keeps blood flowing in the right direction, back to the heart.
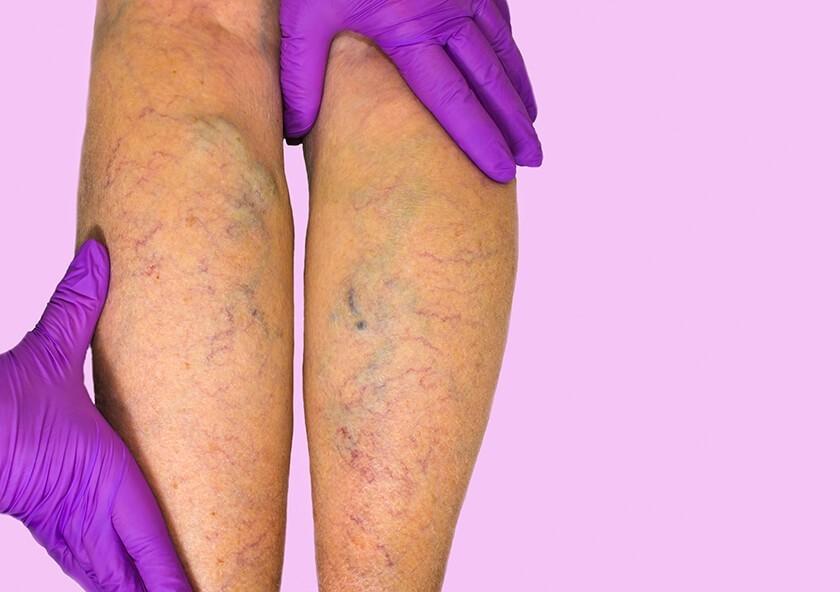
Sometimes, though, those valves can be damaged and they fail to work properly. When that happens, blood collects and becomes sluggish in some areas, especially the feet and lower legs, causing swelling, pain or dull aching, itching, dry or leathery skin, tired legs and hard-to-heal sores. The “backup” of blood also causes the blood pressure inside the lower legs and feet to increase, which in turn causes the vessel walls to weaken and bulge. These are the signs of chronic venous insufficiency, a condition that affects as many as 40 percent of all adults in the U.S.
Risk Factors for CVI
CVI can occur in anyone, but it’s more common among people with specific risk factors, including:
- obesity
- sedentary lifestyles
- occupations that require long periods of standing or sitting
- smoking
- pregnancy
- varicose veins
- deep vein thrombosis (DVT, blood clots located deep in the legs)
DVT is a very common cause of CVI, when a deep clot blocks the normal flow of blood and causes increased pressure in the leg, leading to stress on the valves and, eventually, damage inside the veins. Less commonly, pelvic tumors blood vessel irregularities can cause CVI. Women and people over the age of 50 years are also more likely to have CVI.
In addition to aching and pain in the lower legs, swelling in the ankles and feet, and itchy skin, ulcers that form as a result of CVI can take a long time to heal, leaving you at an increased risk for serious infections, amputations and vasculitis, an inflammation of the blood vessels that can further compromise circulation. Many people only notice the subtler signs of CVI in the warmer months of spring and summer, when shorts and shorter skirts become more common and symptoms like varicose veins or textural changes in the skin become more apparent.
Vascular Ultrasound: The Key to CVI Diagnosis
CVI diagnosis begins with a review of your symptoms as well as your medical history to look for potential risk factors for vein disease. In most cases, your doctor will order a vascular ultrasound, a diagnostic imaging test that plays a central role in the diagnosis and management of CVI. Like other types of ultrasound, vascular ultrasounds use ultrasound energy to create detailed images of the interior of your blood vessels as well as videos of the blood as it flows through your veins.
During the procedure, a special gel will be applied to your skin and the ultrasound’s handheld deice, called a transducer, will be passed slowly over your skin. The transducer releases ultrasound waves which penetrate your skin. The waves cause no pain or sensations of any kind. As the ultrasound waves travel through your skin, they “bounce off” the structures under your skin, including your blood vessels. The transducer recaptures the waves and transmits data about the size and speed of the waves back to a computer. Then, the computer interprets the data to create images of your vessels that can be viewed on a computer monitor. The computer can also calculate how fast your blood is moving to help determine if the vessel is sluggish or narrowed.
The Benefits of Vascular Ultrasound for CVI Management
The “C” in CVI stands for chronic, and that means the disease is ongoing. Managing CVI requires frequent assessments to ensure therapy remains effective to prevent complications. Ultrasound is an ideal choice for assessing CVI because it uses no radiation, which means repeated tests won'[t place you at risk for radiation-related problems. Plus, vascular ultrasound doesn’t require contrast dye, which can take a toll on your kidneys, especially after repeated exposure.
If you have symptoms or risk factors for CVI, it’s important to talk to your doctor about having a vascular evaluation. CVI will not go away on its own – in fact, without prompt medical care, it can get much worse. Seeking treatment as soon as possible is the best way to prevent complications and enjoy a healthier life.