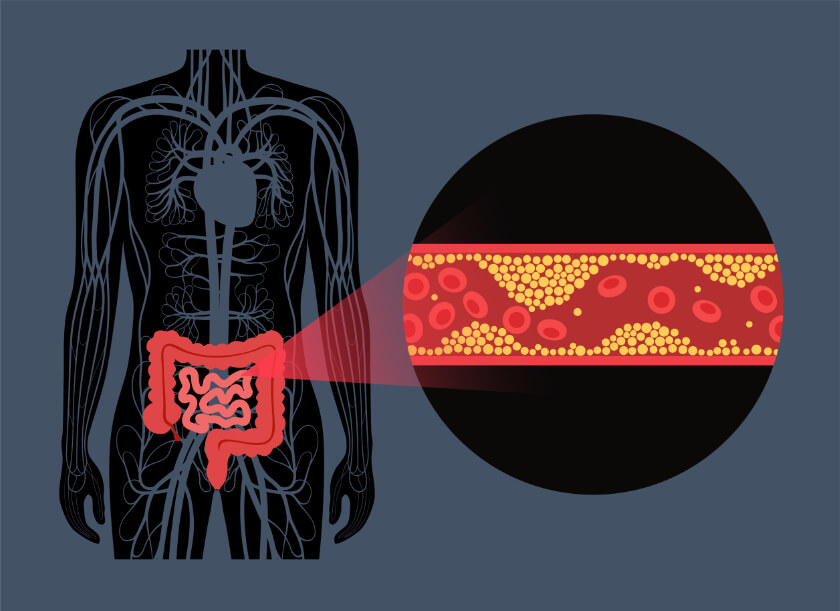
What is Ischemic Colitis?

Schemic colitis is an inflammatory condition affecting the large intestine, also known as the colon or bowel. It develops when there is not enough blood flow to the colon. Ischemic colitis (IC) can be acute, which means it develops and goes away quickly, or it can be a chronic, long-term condition.
Like many other organs, the colon depends on a steady supply of oxygen- and nutrient-rich blood to function correctly. Lack of blood flow to the colon causes inflammation in the affected part of the intestine; without oxygen, cells can die and damage can occur in that part of the intestine.
The word “ischemia” means lack of blood flow, whereas the word “colitis” means inflammation of the lining of the colon. The phrase “ischemic colitis” means inflammation of the colon’s lining due to lack of blood flow to the colon.
Risk Factors for Ischemic Colitis
Certain factors can increase the risk for developing IC. Ischemic colitis risk factors include:
- Age – Ischemic colitis is most common in people over the age of 60, but it can develop at any age, especially in young adults with blood-clotting abnormalities of inflammation of the blood vessels.
- Gender – IC is more common in women.
- Clotting abnormalities – certain health conditions, such as factor V Leiden, can affect the way the blood clots to increase the risk of ischemic colitis.
- High cholesterol – can lead to atherosclerosis, or plaque build-up in the arteries, which prevent blood from flowing properly.
- Reduced blood flow – from low blood pressure, shock, heart failure, or certain other conditions, such as rheumatoid arthritis or diabetes.
- Previous abdominal surgery – scar tissue that forms after an abdominal surgery may reduce blood flow to the colon.
- Heavy exercise – marathon running or other heavy exercise can lead to reduced blood flow to the large intestine.
- Surgery – any surgical procedure involving the aorta, which is the large artery that pumps blood from the heart to the rest of the body.
Symptoms of Ischemic Colitis
People with ischemic colitis often experience abdominal pain, which typically occurs on the left side, but can develop anywhere in the abdomen. The individual typically passes loose stools that are often accompanied by dark clots. Low-grade fevers of 100° F (37.7° C) are common.
Other symptoms of ischemic colitis include:
- Abdominal pain after eating
- Abdominal tenderness
- Feeling an urgent need to have a bowel movement
- Diarrhea
- Vomiting
Potential Complications of Ischemic Colitis
Gangrene, or tissue death, from lack of blood flow to the colon is the most dangerous complication of ischemic colitis. Other complications from IC may include:
- A perforation, or hole, in the colon
- Peritonitis, or inflammation of the tissue lining the abdomen
- Sepsis, which is a very serious condition characterized by widespread bacterial infection
Diagnosis of Ischemic Colitis
Ischemic colitis can be difficult to diagnose, as IC shares many signs and symptoms of other inflammatory bowel conditions, such as Crohn’s disease and ulcerative colitis. It is essential that a doctor rules out acute mesenteric ischemia, a more dangerous condition in which blood flow to the colon is completely and irreversibly blocked.
Diagnosis begins with a review of your medical history and symptoms. Next, the physician will likely order tests and imaging. When inflammation happens, as can happen in a bout of IC, the body floods the affected area with white blood cells to help protect body tissues; blood tests can detect higher white blood cell levels associated with the inflammation.
Doctors usually order computed tomography (CT) scans to detect signs of ischemic colitis. CT scans provide detailed, 3-dimensional images of the colon. They look for signs such as thickening of the intestinal wall, fluid in the peritoneal tissue that lines the abdominal wall, inflammation, or obstructions in the blood vessels that serve the large intestine. Imaging with CT scans can also show signs of ischemia in other organs in the abdomen, such as the liver, kidneys, and spleen. Doctors often order a colonoscopy to inspect the inside of the colon for damage or underlying problems after the large intestine has healed.
Treatment of Ischemic Colitis
Many patients recover from ischemic colitis without treatment, and those with mild cases of IC may not even seek medical treatment. Severe cases require hospitalization, during which patients receive intravenous (IV) fluids to correct any dehydration associated with ischemic colitis and sometimes antibiotics to prevent infection. Sometimes patients require treatment for underlying conditions, such as congestive heart failure or an irregular heartbeat, which may contribute to the development of ischemic colitis. Patients may have to avoid certain medications that constrict blood vessels, such as hormone medications, migraine drugs, and some heart drugs.
Surgery may be necessary in causes of severe symptoms or damage to the bowel. The surgical procedure may involve removing dead tissue, repairing a hole in the colon, or removal of scarred tissue that may be blocking the colon.
For more information about ischemic colitis, consult with a doctor, gastroenterologist, or radiologist.