Everything You Need to Know about Varicose Veins

You probably already know that varicose veins are those twisted and enlarged veins that can appear on the lower legs. You might have already noticed that varicose veins are extremely common too – more than one-third of people in the United States have them, according to the Society for Vascular Surgery. If you are like many people, though, you may think that these unsightly veins are just a cosmetic problem or that you cannot do about them.
The truth is, varicose veins can progress into a more serious problem if left untreated. While there is no cure for varicose veins, there are treatments that reduce their appearance and decrease the risk of complications from these unattractive, dysfunctional veins.
Here is what you need to know about varicose veins and their causes, symptoms, risk factors, prevention strategies and treatments.
About Veins and the Development of Varicose Veins
Veins and arteries are part of the circulatory system. Arteries carry oxygen- and nutrient-rich blood from your heart to the rest of your body. Your body cells use the oxygen and nutrients to carry out various functions, and in the process, create byproducts and toxins. Veins then carry this toxin-rich, oxygen-poor blood back up to your heart.
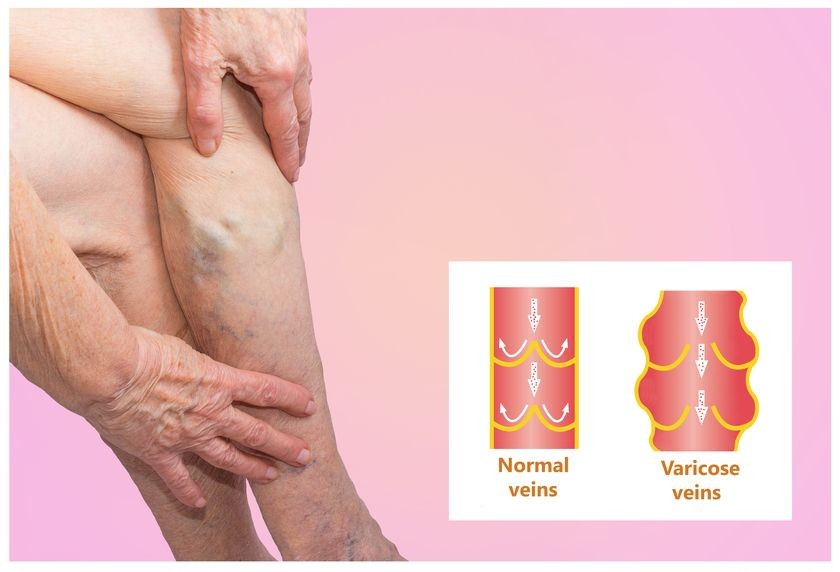
With a little help from gravity, arteries have a relatively easy time moving blood downwards from your heart to your feet. Veins have to work against the force of gravity to move blood back up out of your legs towards your heart. Tiny valves in your veins open and close at just the right time to prevent blood from flowing backwards, or refluxing, in between heartbeats.
After wear and tear over the years, valves can stop functioning properly; the walls of your veins can also become less elastic in time. These effects can allow blood to reflux and accumulate in the veins in your lower legs. Doctors refer to this as chronic venous insufficiency (CVI). Accumulating blood presses against the inside of the veins, and the veins respond by bloating and twisting to become varicose veins.
You can see varicose veins that develop close to the skin; varicose veins can develop deep within your body tissues, so you cannot see them with your naked eye.
Doctors consider varicose veins to be diseased veins, as the veins do a poor job of moving blood up out of your lower legs. This allows the blood, byproducts and toxins to remain in the tissues and prevent them from getting freshly oxygenated blood. In time, this can cause the nearby skin and tissues to break down to cause painful leg sores, known as venous ulcers. Without fresh blood and nutrients, these ulcers can be slow to heal.
The accumulating blood can stagnate in the veins, which may allow blood to clot. Blood clots can move to the lungs, heart or brain to cause serious problems.
Symptoms and Risk Factors of Varicose Veins
In addition to the appearance of bulging, twisted veins, varicose veins that are dark or purple in color may sometimes cause other symptoms. Some but not all people experience an achy or heavy feeling in their legs, for example. Burning, throbbing, cramps or swelling of the lower legs, worsened pain after sitting or standing for a long time, itching near one of the veins, and skin discoloration near a vein may occur.
Certain factors can increase your risk of developing varicose veins. These risk factors include:
- Age – the risk of varicose veins increases with age
- Gender – because of hormone changes during pregnancy, menstruation and menopause, women are more likely to develop varicose veins than are men
- Pregnancy – the volume of blood increases during pregnancy, causing extra pressure on veins
- Family history – if other family members have varicose veins, there is a greater chance that you will too
- Obesity – carrying around excess weight causes additional pressure on veins
- Standing or sitting for long periods – moving around stimulates circulation of blood, whereas sitting or standing in one position allows blood to accumulate
Prevention and Treatment of Varicose Veins
While you cannot completely prevent varicose veins, you can reduce your risk of developing these unsightly veins by:
- Exercising
- Maintaining a healthy weight
- Avoiding tight hosiery and high heels
- Elevating your legs to allow blood to drain from the lower legs
- Changing your position frequently
These same measures can also help treat varicose veins once they develop. Sometimes, though, these measures are not enough to reduce the appearance and effects of varicose veins. Fortunately, vein doctors provide a wide variety of varicose vein treatments
Treatment begins with a thorough evaluation of your veins. This evaluation may include the use of duplex ultrasound, a technology that uses sound waves to create an image of your veins. Your doctor uses the information from the ultrasound and evaluation to recommend treatment.
Varicose vein treatments usually focus on making the disease vein swell and close permanently. The body routes blood to other veins. The treated vein eventually breaks apart and nearby tissue absorbs the remnants.
Today’s varicose vein treatments are minimally invasive and do not require an overnight stay at a hospital. These treatments include endovenous laser ablation (EVLA), which uses the light energy of a laser, and other types of ablation that use heat or chemicals to close the diseased veins.
For more information about varicose veins and their treatment, consult with your doctor or vein specialist. Treatment can reduce the appearance of these bulging veins and restore the youthful look of your lower legs.