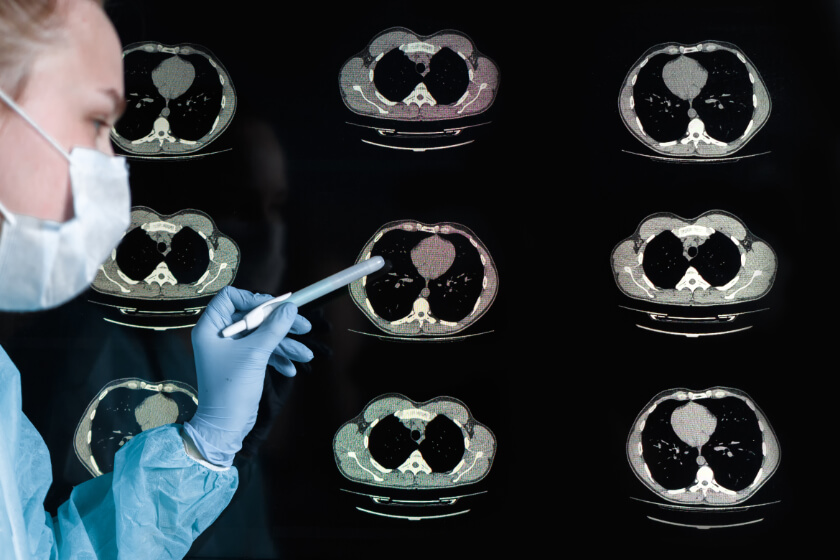
What Does COVID-19 Look Like on a CT Scan?

If you have COVID-19, your doctor might order a CT scan. Have you ever wondered what doctors look for when they review the results of the CT scan?
COVID-19 typically causes fever, shortness of breath, and cough. Doctors usually order blood tests, such as PCR and antigen testing, to diagnose the disease. They also use imaging technology, such as computed tomography (CT) scans, to help diagnose and treat COVID-19.
Coronavirus, which is the virus that causes COVID-19, moves down the respiratory tract to affect the mouth, nose, throat, and lungs. The virus has spiky surface proteins that latch onto receptors on healthy cells, and especially onto the receptors in lung cells. Once attached to the cell receptors, the virus takes command of lung cells to cause inflammation that makes it hard to breathe. Inflammation can cause pneumonia, which is an infection of the small air sacs (alveoli) that exchanges oxygen and carbon dioxide. The infection causes the alveoli to fill up with pus or fluid, which makes it hard to breathe.
The coronavirus infection can also cause other changes to the respiratory tract to make breathing difficult. For example, coronavirus can affect the bronchi, which are the tubes that connect the windpipe and the lungs. Lung problems associated with COVID-19 can also prevent the alveoli from absorbing oxygen, which can lead to low levels of oxygen in the blood, known as hypoxemia.
COVID-19 can cause mild, severe, or even critical illness, depending on how much coronavirus has affected the lungs. CT scans capture images of the alveoli, bronchi, and other parts of the respiratory tract to help doctors assess the effects COVID-19 is having on patients’ lungs. The CT images can help doctors determine which parts of the lung are involved, assess the severity of an infection, and even predict whether the patient is getting better or worse.
CT Scans Show Signs of COVID-19
A CT scan is a medical imaging technique that uses a combination of multiple x-ray images and a computer to create pictures of tissues inside the human body. In an x-ray, bones and other dense tissue appear as white areas, while gasses, liquids, and empty spaces are black; other tissues appear gray, depending on their density. In a normal lung CT, then, the lungs appear as large black areas. To determine the extent of lung involvement in patients with COVID-19, radiologists and other doctors look for areas of gray on the CT images. Doctors also look for specific patterns of gray and white appearing in the image or changes to specific structures within the respiratory tract.
Ground glass opacities
As its name suggests, ground glass opacity looks like bits of ground glass scattered about the lungs. These gray areas are opaque, which means they are not transparent. The ground glass opacities are multifocal and bilateral, which means several gray spots may appear in each lung. Ground glass opacities may appear in the central inner part of the lungs or in the peripheral outer part of the lungs.
Ground glass opacities are the most common finding in CT scans of people with COVID-19, appearing in up to 98 percent of cases.
Crazy paving
Crazy paving is a linear pattern superimposed over a ground glass opacity background to create the appearance of irregular, or “crazy,” paving stones. Fluid in the tiny air sacs of the lungs, known as alveolar edema, and inflammation can cause the crazy paving patterns seen in CT scans of the lungs. Crazy paving is often a sign that COVID-19 is progressing, or getting worse.
Consolidation
Consolidation occurs when fluid, such as pus, blood or water, fills up the airways in the lungs. It can be multifocal, patchy, or appear in different sections of the lungs. Consolidation can co-exist with ground glass opacities; it can also be a sign that COVID-19 is progressing.
Vascular dilation
Coronavirus infection can widen, or dilate, the blood vessels of the lungs; doctors can see these dilated blood vessels on CT scan images. This condition, known as vascular dilation, usually appears in the area of ground glass opacities. Vascular dilation appears to play a role in hypoxemia in patients with COVID-19-related pneumonia.
Reticular pattern
Reticular patterns are a collection of small linear opacities that resemble a net. They develop as the result of thickening of the interstitial structures, which are lace-like network of tissue that supports the air sacs in the lungs. Thickening of these structures prevents the air sacs from filling with air, which makes it hard to breathe in.
The net-like pattern can be fine, medium, or coarse. The lines in fine reticular patterns are very thin, measuring 1-2 mm; medium reticular patterns look a bit like honeycombs and measure 3 – 10 mm. Coarse reticular patterns measure greater than 10 mm, and usually indicate a severe lung problem. Reticular patterns are common in patients with COVID, and the appearance of reticular patterns tends to increase in prolonged cases of COVID-19.
Traction bronchiectasis
Traction bronchiectasis causes inflammation and dilation of the bronchial tissue, and thickens the bronchi in a way that makes it harder to inhale and to cough out phlegm and sputum. In time, the condition can destroy the bronchi.
CT scans help doctors provide better care for their patients with COVID-19 infections. Based on what they find in CT scans, doctors can create treatment plans that help patients get well.